Quality Improvement
Category: Quickshot Oral Session 15
Quickshot Oral : Quickshot Oral Session 15
MOVE THE LINE: STANDARIZATION OF MIDLINE PLACEMENT AND MANAGEMENT DECREASES VENOUS ACCESS COMPLICATIONS IN THE INTENSIVE CARE UNIT SETTING
Monday, February 13, 2023
7:00am - 8:00am East Coast USA Time
- JW
Jennifer Whittington, MD, PhD
General Surgeon
Mount Sinai, United States - JW
Jennifer Whittington, MD, PhD
General Surgeon
Mount Sinai, United States
Presenter(s)
Principal Contact(s)
Objectives: Midline insertion is a peripheral venous access frequently performed in the ICU. Substantial morbidity, mortality, length of stay, cost of care, and quality of life can result from immediate complications (IC) and delayed complications (DC) secondary to midline insertion, particularly in a critically ill population. The aim of this study is to IC ( < 10 days) and DC (>10 days) after midline placement with a standardized approach in a closed surgical intensive care unit (cSICU).
Methods: All midline insertions in a cSICU were performed with a standardized protocol by protocol trained ICU providers from January 1, 2021 through January 1, 2022. All complications after midline insertion were recorded and reviewed by the SICU program director. Statistical analysis included qualitative analysis, Spearman rank correlation coefficient to compare non-parametric variables, and log-linear regression modeling to analyze associations between immediate and delayed midline complications.
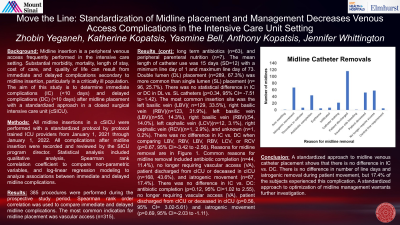
Results: 385 procedures were performed. The most common indication was vascular access (n=315), long term antibiotics (n=63), peripheral parenteral nutrition (n=7). The mean length of catheter use was 15 days (SD=12). Double lumen (DL) placement (n=289, 67.3%) was more common than single lumen (SL) (n= 96, 25.7%). There was no statistical difference in IC or DC in DL vs. SL catheters (p=0.34, 95% CI= -7.51 to−1.42). The most common insertion site was left basilic vein (LBV)( n=129, 33.5%), right basilic vein (RBV)(n=123, 31.9%), left basilic vein (LBV)(n=55, 14.3%), right basilic vein (RBV)(54, 14.0%), left cephalic vein (LCV)(n=12, 3.1%), right cephalic vein (RCV)(n=1, 2.9%), and unknown (n=1, 0.2%). There was no difference in IC vs. DC when comparing LBV, RBV, LBV, RBV, LCV, or RCV (p=0.67, 95% CI=-3.42 to -2.56). Reasons for midline removal are in Figure 1. Common reasons for midline removal included antibiotic completion (n=44, 11.4%), no longer requiring vascular access (VA), patient discharged from cICU or deceased in cICU (n=168, 43.6%), and iatrogenic movement (n=67, 17.4%). There was no difference in IC vs. DC: antibiotic completion (p=0.12, 95% CI=1.02 to 2.55), no longer requiring vascular access (VA), patient discharged from cICU or deceased in cICU (p=0.56, 95% CI= 3.02-5.61) and iatrogenic movement (p=0.69, 95% CI=-2.03 to -1.11).
Conclusion: A standardized approach to midline venous catheter placement shows that there is no difference in IC vs. DC. There is no difference in number of line days and iatrogenic removal during patient movement, but 17.4% of the subjects experienced this complication. A standardized approach to optimization of midline management warrants further investigation.
Methods: All midline insertions in a cSICU were performed with a standardized protocol by protocol trained ICU providers from January 1, 2021 through January 1, 2022. All complications after midline insertion were recorded and reviewed by the SICU program director. Statistical analysis included qualitative analysis, Spearman rank correlation coefficient to compare non-parametric variables, and log-linear regression modeling to analyze associations between immediate and delayed midline complications.
Results: 385 procedures were performed. The most common indication was vascular access (n=315), long term antibiotics (n=63), peripheral parenteral nutrition (n=7). The mean length of catheter use was 15 days (SD=12). Double lumen (DL) placement (n=289, 67.3%) was more common than single lumen (SL) (n= 96, 25.7%). There was no statistical difference in IC or DC in DL vs. SL catheters (p=0.34, 95% CI= -7.51 to−1.42). The most common insertion site was left basilic vein (LBV)( n=129, 33.5%), right basilic vein (RBV)(n=123, 31.9%), left basilic vein (LBV)(n=55, 14.3%), right basilic vein (RBV)(54, 14.0%), left cephalic vein (LCV)(n=12, 3.1%), right cephalic vein (RCV)(n=1, 2.9%), and unknown (n=1, 0.2%). There was no difference in IC vs. DC when comparing LBV, RBV, LBV, RBV, LCV, or RCV (p=0.67, 95% CI=-3.42 to -2.56). Reasons for midline removal are in Figure 1. Common reasons for midline removal included antibiotic completion (n=44, 11.4%), no longer requiring vascular access (VA), patient discharged from cICU or deceased in cICU (n=168, 43.6%), and iatrogenic movement (n=67, 17.4%). There was no difference in IC vs. DC: antibiotic completion (p=0.12, 95% CI=1.02 to 2.55), no longer requiring vascular access (VA), patient discharged from cICU or deceased in cICU (p=0.56, 95% CI= 3.02-5.61) and iatrogenic movement (p=0.69, 95% CI=-2.03 to -1.11).
Conclusion: A standardized approach to midline venous catheter placement shows that there is no difference in IC vs. DC. There is no difference in number of line days and iatrogenic removal during patient movement, but 17.4% of the subjects experienced this complication. A standardized approach to optimization of midline management warrants further investigation.

