Trauma
Category: Quickshot Oral Session 18
Quickshot Oral : Quickshot Oral Session 18
GENDER-BASED FRAILTY IN MULTIPLE ORTHOPEDIC FRACTURES
Monday, February 13, 2023
7:00am - 8:00am East Coast USA Time
- MG
Michelle E. Gary, MD
General Surgery Resident PGY2
University of Illinois COM Peoria, United States - FB
Faran Bokhari, MD
United States
Presenter(s)
Principal Contact(s)
Objectives: The 5-factor modified frailty index (mFI-5) has been shown to be an excellent comorbidity-based risk stratification tool for trauma outcomes and disposition, but it has not previously been used to identify patients at risk for multiple fractures. The aim of this study was to determine whether mFI-5 is a better predictor than age for the risk of combined femur-humerus fractures compared to femur fractures alone.
Methods: We retrospectively analyzed the (2017-2019) ACS-TQIP database to identify patients > 65 years-old with femur and combined femur-humerus fractures using the ICD-10 code. Patients with major injuries to other organs (AIS >3) were excluded. The mFI-5 score was then calculated and categorized as no frailty (mFI-5 = 0), low frailty (mFI-5 = 1-2), intermediate frailty (mFI-5 = 3), and severe frailty (mFI-5 = 4-5). Univariate analysis was performed adjusting for age, gender, race, GCS, ISS, vital signs, and comorbidities. Multivariate logistic regression was performed adjusting for steroid use, dementia, mental/personality disorders, and anticoagulation. All statistical analyses were performed using SPSS with a 95% confidence interval.
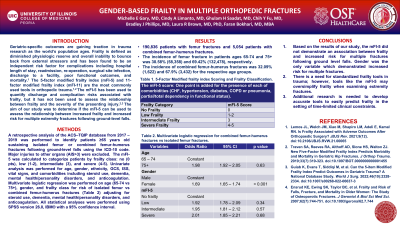
Results: A total of 190,836 patients with femur fractures and 5,054 patients with combined femur-humerus fractures were identified. The incidence of femur fracture in patients ages 65-74 and 75+ was 30.58% (58,358) and 69.42% (132,478), while the incidence of combined femur-humerus fractures was 32.09% (1,622) and 67.9% (3,432), respectively. Patients 75+ years-old did not have a statistically significant odds ratio for combined femur-humerus fractures (OR 1.98, 95% CI [1.92, 2.05], p = 0.63) compared to patients 65-74 years-old. Sub-analysis of patients by mFI-5 scores demonstrated no statistically significant increased risk for combined fractures except in the low frailty group (OR 1.02, 95% CI [1.6, 1.85], p < 0.001). Older females (>75 years-old) had higher risk of combined femur-humerus fractures (OR 1.69, 95% CI [1.65, 1.74], p < 0.001) compared to males.
Conclusion: While frailty indices such as the mFI-5 are excellent at predicting post-injury outcomes; gender-based frailty is a stronger predictor of which patients are at higher risk of multiple long bone fractures. Prevention strategies should target gender-based populations given increased burden of care with multiple injuries.
Methods: We retrospectively analyzed the (2017-2019) ACS-TQIP database to identify patients > 65 years-old with femur and combined femur-humerus fractures using the ICD-10 code. Patients with major injuries to other organs (AIS >3) were excluded. The mFI-5 score was then calculated and categorized as no frailty (mFI-5 = 0), low frailty (mFI-5 = 1-2), intermediate frailty (mFI-5 = 3), and severe frailty (mFI-5 = 4-5). Univariate analysis was performed adjusting for age, gender, race, GCS, ISS, vital signs, and comorbidities. Multivariate logistic regression was performed adjusting for steroid use, dementia, mental/personality disorders, and anticoagulation. All statistical analyses were performed using SPSS with a 95% confidence interval.
Results: A total of 190,836 patients with femur fractures and 5,054 patients with combined femur-humerus fractures were identified. The incidence of femur fracture in patients ages 65-74 and 75+ was 30.58% (58,358) and 69.42% (132,478), while the incidence of combined femur-humerus fractures was 32.09% (1,622) and 67.9% (3,432), respectively. Patients 75+ years-old did not have a statistically significant odds ratio for combined femur-humerus fractures (OR 1.98, 95% CI [1.92, 2.05], p = 0.63) compared to patients 65-74 years-old. Sub-analysis of patients by mFI-5 scores demonstrated no statistically significant increased risk for combined fractures except in the low frailty group (OR 1.02, 95% CI [1.6, 1.85], p < 0.001). Older females (>75 years-old) had higher risk of combined femur-humerus fractures (OR 1.69, 95% CI [1.65, 1.74], p < 0.001) compared to males.
Conclusion: While frailty indices such as the mFI-5 are excellent at predicting post-injury outcomes; gender-based frailty is a stronger predictor of which patients are at higher risk of multiple long bone fractures. Prevention strategies should target gender-based populations given increased burden of care with multiple injuries.

