Trauma
Category: Quickshot Oral Session 09
Quickshot Oral : Quickshot Oral Session 09
INCIDENCE OF ADULT TRAUMATIC INTRACRANIAL BLEEDING AND LIKELIHOOD OF ROUTINE DISCHARE: DO CO-MORBIDITIES MATTER?
Sunday, February 12, 2023
7:00am - 8:00am East Coast USA Time
- YP
Yelena Pecheny, MD
PGY1
HCA Healthcare - HR
Heather Rhodes, Rhodes, PhD
Trauma Research Specialist
Grand Strand Medical Center, United States
Presenter(s)
Principal Contact(s)
Objectives: The current literature does not readily address the morbidity, associated functional outcomes, and comorbidities of those who survive intracranial hemorrhage.
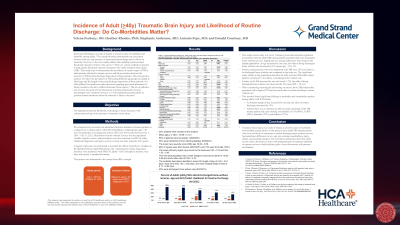
Methods: This is a single-center study of Trauma Registry data, from July 1, 2016, to October 31, 2021. The inclusion criteria were based upon age (≥40 years) and ICD10 diagnosis of an ICH. Disposition to home without services was the dependent variable. A logistic regression was performed to ascertain the effects of predictor variables on the likelihood that an adult ICH trauma patient experienced a routine disposition.
Results: 2031 patients were included in the analysis based upon the requirements specified in the methods section; 837 (41%) experienced routine discharge to home without services. The logistic regression model was statistically significant (N=1905, p< 0.01). Several significant increases in routine discharge odds were identified, including increasing Glasgow Coma Score (OR=1.10, p=0.01). Additional factors in the reduction of odds for routine discharge included increasing age (OR=0.94, p< 0.01); females (OR=0.75, p=0.02); increasing ISS (OR=0.92, p< 0.01); increasing length of stay
(OR=0.85, p< 0.01); full activation (OR-0.59, p=0.01); and pre-existing comorbidities CVA (OR=0.51, p=0.01); COPD (OR=0.54, p=0.01); Dementia (OR=0.55, p< 0.01); and Diabetes (OR=0.73, p=0.04).
Conclusion: The likelihood of discharge to home decreases (by 6%) with the advancement of age (per year) in the presence of intracranial hemorrhage. This evidence, along with additional risk from specific pre-existing comorbidities, may aid clinical decision-making in care discussions with patients and families.
Methods: This is a single-center study of Trauma Registry data, from July 1, 2016, to October 31, 2021. The inclusion criteria were based upon age (≥40 years) and ICD10 diagnosis of an ICH. Disposition to home without services was the dependent variable. A logistic regression was performed to ascertain the effects of predictor variables on the likelihood that an adult ICH trauma patient experienced a routine disposition.
Results: 2031 patients were included in the analysis based upon the requirements specified in the methods section; 837 (41%) experienced routine discharge to home without services. The logistic regression model was statistically significant (N=1905, p< 0.01). Several significant increases in routine discharge odds were identified, including increasing Glasgow Coma Score (OR=1.10, p=0.01). Additional factors in the reduction of odds for routine discharge included increasing age (OR=0.94, p< 0.01); females (OR=0.75, p=0.02); increasing ISS (OR=0.92, p< 0.01); increasing length of stay
(OR=0.85, p< 0.01); full activation (OR-0.59, p=0.01); and pre-existing comorbidities CVA (OR=0.51, p=0.01); COPD (OR=0.54, p=0.01); Dementia (OR=0.55, p< 0.01); and Diabetes (OR=0.73, p=0.04).
Conclusion: The likelihood of discharge to home decreases (by 6%) with the advancement of age (per year) in the presence of intracranial hemorrhage. This evidence, along with additional risk from specific pre-existing comorbidities, may aid clinical decision-making in care discussions with patients and families.

