Trauma
Category: Quickshot Oral Session 23
Quickshot Oral : Quickshot Oral Session 23
REPAIR OF TRAUMATIC SPIGELIAN HERNIA WITH ROBOTIC ASSIST
Tuesday, February 14, 2023
7:00am - 8:00am East Coast USA Time

William M. Hudson, MD
Resident
Atlanta Medical Center, United States- gc
gregory coffman, MD
United States
Presenter(s)
Principal Contact(s)
Objectives: Traumatic abdominal wall hernias (TAWH) are a rare occurrence. Originally described as ‘herniation through disrupted musculature and fascia, associated with adequate trauma, without skin penetration and no evidence of a prior hernia defect at the site of injury’ the injury carries with it concerns for concomitant as well as occult injuries. Occurring at the semilunar line of the anterior abdominal wall, spigelian hernias are also rare. Similar to femoral hernias, they carry a high incarceration incidence. Our case combines these 2 rare occurrences.
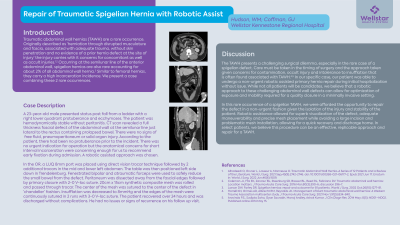
A 23-year-old male presented status post fall from ladder with a right lower quadrant protuberance and ecchymoses. The patient was hemodynamically stable without peritonitis. CT scan revealed a full thickness fascial defect of the abdominal wall at the semilunar line lateral to the rectus containing prolapsed bowel. There were no signs of free fluid, pneumoperitoneum or solid organ injury. No prior hernia was reported. There was no urgent indication for operation but the anatomical concerns for short interval incarceration were concerning enough for us to recommend early fixation during admission. A robotic assisted approach was chosen.
In the OR, a LUQ 8mm port was placed using direct vision trocar technique followed by 2 additional trocars in the mid and lower left abdomen. The patient was then positioned left side down in Trendelenburg. Fenestrated bipolar and atraumatic forceps were used to safely reduce the small bowel from the defect. Peritoneum was dissected away from the fascial edges followed by primary closure with 2-0 V-loc suture. 20cm x 15cm synthetic composite mesh was rolled and passed through trocar. The center of the mesh was suture to the center of the defect in ‘chandelier’ fashion. Insufflation was decreased to 8mmHg and the edges of the mesh were continuously sutured in 2 runs with 3-0 V-loc suture. The patient recovered over 24 hours and was discharged without complications. He had no issues or signs of recurrence on his follow up visit.
In this rare occurrence of a spigelian TAWH, we were afforded the opportunity to repair the defect in a non-urgent fashion given the isolation of the injury and stability of the patient. Robotic assistance allowed for superb visualization of the defect, adequate maneuverability and precise mesh placement while avoiding a large incision and problematic mesh installation, allowing for a quick recovery and discharge home. In select patients, this procedure can be an effective, replicable approach and repair for a TAWH.
Methods:
Results:
Conclusion:
A 23-year-old male presented status post fall from ladder with a right lower quadrant protuberance and ecchymoses. The patient was hemodynamically stable without peritonitis. CT scan revealed a full thickness fascial defect of the abdominal wall at the semilunar line lateral to the rectus containing prolapsed bowel. There were no signs of free fluid, pneumoperitoneum or solid organ injury. No prior hernia was reported. There was no urgent indication for operation but the anatomical concerns for short interval incarceration were concerning enough for us to recommend early fixation during admission. A robotic assisted approach was chosen.
In the OR, a LUQ 8mm port was placed using direct vision trocar technique followed by 2 additional trocars in the mid and lower left abdomen. The patient was then positioned left side down in Trendelenburg. Fenestrated bipolar and atraumatic forceps were used to safely reduce the small bowel from the defect. Peritoneum was dissected away from the fascial edges followed by primary closure with 2-0 V-loc suture. 20cm x 15cm synthetic composite mesh was rolled and passed through trocar. The center of the mesh was suture to the center of the defect in ‘chandelier’ fashion. Insufflation was decreased to 8mmHg and the edges of the mesh were continuously sutured in 2 runs with 3-0 V-loc suture. The patient recovered over 24 hours and was discharged without complications. He had no issues or signs of recurrence on his follow up visit.
In this rare occurrence of a spigelian TAWH, we were afforded the opportunity to repair the defect in a non-urgent fashion given the isolation of the injury and stability of the patient. Robotic assistance allowed for superb visualization of the defect, adequate maneuverability and precise mesh placement while avoiding a large incision and problematic mesh installation, allowing for a quick recovery and discharge home. In select patients, this procedure can be an effective, replicable approach and repair for a TAWH.
Methods:
Results:
Conclusion:

