Trauma
Category: Quickshot Oral Session 24
Quickshot Oral : Quickshot Oral Session 24
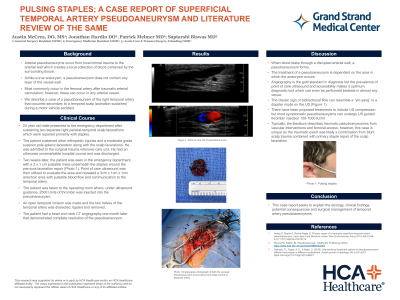
PULSING STAPLES; A CASE REPORT OF SUPERFICIAL TEMPORAL ARTERY PSEUDOANEURYSM AND LITERATURE REVIEW OF THE SAME.
Tuesday, February 14, 2023
7:00am - 8:00am East Coast USA Time
- AM
Austin O. McCrea, DO (he/him/his)
Resident
Grand Strand Medical Center, United States - SB
Saptarshi Biswas, MD FACS
Attending, United States
Presenter(s)
Principal Contact(s)
Objectives: Arterial pseudoaneuryms occur from local intimal trauma to the arterial wall which creates a local collection of blood contained by the surrounding tissue. Unlike a true aneurysm, a pseudoaneurysm does not contain any layer of the vessel wall. These most commonly occur in the femoral artery after traumatic arterial cannulation; however, these can occur in any arterial vessel. We describe a case of a pseudoaneurysm of the right temporal artery that occurred secondary to a temporal scalp laceration sustained during a motor vehicle accident. This 24 year old male presented to the emergency department after sustaining two separate right parietal-temporal scalp lacerations which were repaired primarily with staples. The patient sustained other orthopedic injuries and a moderate grade superior pole splenic laceration along with the scalp lacerations. He was admitted to the surgical trauma intensive care unit. He had an otherwise unremarkable hospital course and was discharged. Two weeks later, the patient was seen in the emergency department with a 2 x 1 cm pulsatile mass underneath the staples around the previous laceration repair. Point of care ultrasound was then utilized to evaluate the area and revealed a 3cm x 1cm x 1cm anechoic area with pulsatile blood flow and communication to the temporal artery. The patient was taken to the operating room where, under ultrasound guidance, 2500 Units of thrombin was injected into the pseudoaneurysm. Then, an open temporal incision was made and the two halves of the temporal artery was dissected, ligated and removed. The patient had a head and neck CT angiography one month later that demonstrated complete resolution of the pseudoaneurysm. This case report seeks to explain the etiology, clinical findings, potential consequences and surgical management of temporal artery pseudoaneurysms with a review of the pertinent literature.
Methods:
Results:
Conclusion:
Methods:
Results:
Conclusion:

