Trauma
Category: Quickshot Oral Session 06
Quickshot Oral : Quickshot Oral Session 06
BUG JUICE AND CHEST TUBES: ARE PROPHYLACTIC ANTIBIOTICS NEEDED FOR TUBE THORACOSTOMY PLACEMENT?
Saturday, February 11, 2023
3:00pm - 4:00pm East Coast USA Time

Morgan L. Brown, MD (she/her/hers)
Resident
LSUHSC - New Orleans , United States- AS
Alison Smith, MD
United States
Presenter(s)
Principal Contact(s)
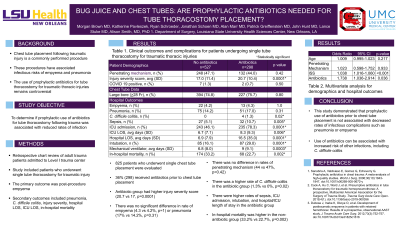
Objectives: Chest tube placement following traumatic injury is one of the most common procedures performed. Despite the routine nature of performing these procedures, there are associated infectious risks of empyema and pneumonia. The use of prophylactic antibiotics prior to tube thoracostomy for traumatic thoracic injuries remains controversial with conflicting literature to support this practice. The purpose of this study was to determine if prophylactic use of antibiotics for tube thoracostomy following trauma was associated with reduced rates of infection.
Methods: This study is a retrospective chart review of adult patients at a Level 1 Trauma Center from July 1, 2012-January 31, 2022 with thoracic injuries requiring tube thoracostomy. The primary outcome was post-procedure empyema. Secondary outcomes included the incidence of pneumonia, C. diff colitis, injury severity, hospital length of stay (LOS), ICU LOS, and in-hospital mortality. Empyema was defined by positive pleural cultures. Pneumonia was defined by positive sputum cultures and radiographic evidence. Results were compared using univariate analysis with p< 0.05 considered significant.
Results: 827 patients who underwent placement of a single chest tube were included in the study. Of these, 36% (n=298/827) received antibiotics prior to chest tube placement. The antibiotic group had significantly higher injury severity scores, (20.7 vs 17, p=0.0001). There was no difference in rates of penetrating mechanism between the groups, (44 vs 47%, p=0.42). There was no difference in rates of empyema (4.3% vs 4.2%, p=1.0) or pneumonia (17% vs 14.2% p=0.31) for the group who received antibiotics prior to tube thoracostomy. There were significantly more patients with C. diff colitis in the antibiotics group (1.3% vs 0%, p=0.02). Patients in the antibiotics group had significantly higher rates of sepsis (10.7% vs 5.1%, p=0.005), ICU admission (78.3% vs 46.1%, p=0.0001), intubation (29% vs 16.1%, p=0.0001), and longer hospital (16.5 vs 6.9, p=0.0001) and ICU length of stay (8.3 vs 6.7, p=0.006). In-hospital mortality was higher in the non-antibiotic group (33.2% vs 22.7%, p=0.002).
Conclusion: Prophylactic use of antibiotics prior to chest tube placement is not associated with decreased rates of infectious complications such as empyema or pneumonia and can have deleterious effects associated with their use such as increased risk of C. diff infections. Future prospective studies focused on evidence-based guideline development are needed.
Methods: This study is a retrospective chart review of adult patients at a Level 1 Trauma Center from July 1, 2012-January 31, 2022 with thoracic injuries requiring tube thoracostomy. The primary outcome was post-procedure empyema. Secondary outcomes included the incidence of pneumonia, C. diff colitis, injury severity, hospital length of stay (LOS), ICU LOS, and in-hospital mortality. Empyema was defined by positive pleural cultures. Pneumonia was defined by positive sputum cultures and radiographic evidence. Results were compared using univariate analysis with p< 0.05 considered significant.
Results: 827 patients who underwent placement of a single chest tube were included in the study. Of these, 36% (n=298/827) received antibiotics prior to chest tube placement. The antibiotic group had significantly higher injury severity scores, (20.7 vs 17, p=0.0001). There was no difference in rates of penetrating mechanism between the groups, (44 vs 47%, p=0.42). There was no difference in rates of empyema (4.3% vs 4.2%, p=1.0) or pneumonia (17% vs 14.2% p=0.31) for the group who received antibiotics prior to tube thoracostomy. There were significantly more patients with C. diff colitis in the antibiotics group (1.3% vs 0%, p=0.02). Patients in the antibiotics group had significantly higher rates of sepsis (10.7% vs 5.1%, p=0.005), ICU admission (78.3% vs 46.1%, p=0.0001), intubation (29% vs 16.1%, p=0.0001), and longer hospital (16.5 vs 6.9, p=0.0001) and ICU length of stay (8.3 vs 6.7, p=0.006). In-hospital mortality was higher in the non-antibiotic group (33.2% vs 22.7%, p=0.002).
Conclusion: Prophylactic use of antibiotics prior to chest tube placement is not associated with decreased rates of infectious complications such as empyema or pneumonia and can have deleterious effects associated with their use such as increased risk of C. diff infections. Future prospective studies focused on evidence-based guideline development are needed.

