General Surgery
Category: Quickshot Oral Session 19
Quickshot Oral : Quickshot Oral Session 19
NON-ROTATION OF THE INTESTINES AND SUGAR SPLEEN IN A POST-CABG PATIENT
Monday, February 13, 2023
7:00am - 8:00am East Coast USA Time

Evan L. Barrios, MD
Resident
University of Florida, United States- JT
Jessica E. Taylor, MD, MBA
Assistant Professor
University of Florida, United States
Presenter(s)
Principal Contact(s)
Objectives: INTRODUCTION
Intestinal non-rotation and perisplenitis are two rarely seen entities which were encountered in the same acutely decompensating patient, and, while unrelated, highlight the importance of recognizing variations in anatomy and understanding the clinical significance of rare disease processes.
Intestinal malrotation most commonly presents in childhood (incidence 0.02%-1%), with adult presentation making up 0.5% of all cases. Embryologic intestinal rotation occurs in three stages. In non-rotation, the midgut fails to rotate secondary to umbilical ring laxity. The large intestine ultimately lies in the patient’s left hemi-abdomen with the small intestine on the right without Ladd’s bands as seen in malrotation.
CASE DESCRIPTION
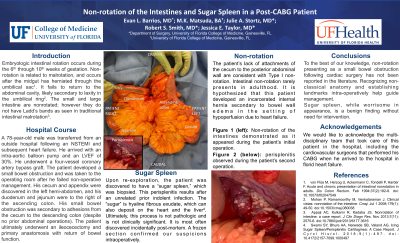
The patient was a 78-year-old male without prior abdominal surgeries who presented in acute heart failure after a myocardial infarction. He underwent a four-vessel coronary artery bypass graft (CABG) operation complicated by small bowel obstruction. Upon abdominal exploration, non-rotation of the intestines was encountered with adhesions from the cecum to the descending colon creating an internal hernia with incarcerated small intestine. Following adhesiolysis and reduction of the hernia, the patient underwent temporary abdominal closure. During re-exploration, patchy ischemia of the terminal ileum and cecum was noted, and an ileocolic resection with primary anastomosis was performed with subsequent return of bowel function. It was also discovered upon exploration that the patient had a “sugar spleen” which was biopsied.
DISCUSSION
The patient’s lack of attachments of the cecum to the posterior abdominal wall are consistent with Type I non-rotation. However, he did have significant inter-colonic adhesions which led to the internal hernia. Intestinal non-rotation can present emergently during primary obstruction, chronically with persistent abdominal pain, or incidentally during an unrelated operation. In this patient, a small bowel obstruction developed via internal hernia secondary to his cardiovascular pathology. It is hypothesized that bowel edema secondary to hypoperfusion in the setting of heart failure and open-heart surgery contributed to his acute obstruction.
In addition, the patient was discovered to have perisplenitis during exploration, which consists of hyaline fibrous exudates which coat the spleen (also known as “icing sugar spleen”). This process is not pathologic and carries little clinical significance, although its appearance during exploration in an unstable patient could raise concern if one is unfamiliar with this pathology.
This case demonstrates a cause of incarcerated small intestine following a CABG which has not previously been reported in the literature. Perisplenitis, while impressive-appearing, is a benign condition which does not warrant further workup.
Methods:
Results:
Conclusion:
Intestinal non-rotation and perisplenitis are two rarely seen entities which were encountered in the same acutely decompensating patient, and, while unrelated, highlight the importance of recognizing variations in anatomy and understanding the clinical significance of rare disease processes.
Intestinal malrotation most commonly presents in childhood (incidence 0.02%-1%), with adult presentation making up 0.5% of all cases. Embryologic intestinal rotation occurs in three stages. In non-rotation, the midgut fails to rotate secondary to umbilical ring laxity. The large intestine ultimately lies in the patient’s left hemi-abdomen with the small intestine on the right without Ladd’s bands as seen in malrotation.
CASE DESCRIPTION
The patient was a 78-year-old male without prior abdominal surgeries who presented in acute heart failure after a myocardial infarction. He underwent a four-vessel coronary artery bypass graft (CABG) operation complicated by small bowel obstruction. Upon abdominal exploration, non-rotation of the intestines was encountered with adhesions from the cecum to the descending colon creating an internal hernia with incarcerated small intestine. Following adhesiolysis and reduction of the hernia, the patient underwent temporary abdominal closure. During re-exploration, patchy ischemia of the terminal ileum and cecum was noted, and an ileocolic resection with primary anastomosis was performed with subsequent return of bowel function. It was also discovered upon exploration that the patient had a “sugar spleen” which was biopsied.
DISCUSSION
The patient’s lack of attachments of the cecum to the posterior abdominal wall are consistent with Type I non-rotation. However, he did have significant inter-colonic adhesions which led to the internal hernia. Intestinal non-rotation can present emergently during primary obstruction, chronically with persistent abdominal pain, or incidentally during an unrelated operation. In this patient, a small bowel obstruction developed via internal hernia secondary to his cardiovascular pathology. It is hypothesized that bowel edema secondary to hypoperfusion in the setting of heart failure and open-heart surgery contributed to his acute obstruction.
In addition, the patient was discovered to have perisplenitis during exploration, which consists of hyaline fibrous exudates which coat the spleen (also known as “icing sugar spleen”). This process is not pathologic and carries little clinical significance, although its appearance during exploration in an unstable patient could raise concern if one is unfamiliar with this pathology.
This case demonstrates a cause of incarcerated small intestine following a CABG which has not previously been reported in the literature. Perisplenitis, while impressive-appearing, is a benign condition which does not warrant further workup.
Methods:
Results:
Conclusion:

